Candidiasis
Candidiasis is a fungal infection caused by yeasts
that belong to the genus Candida.
that belong to the genus Candida.
There are over 20 species of Candida yeasts that can cause infection in humans, the most common of which is Candida albicans.
Candida yeasts normally live on the skin and mucous membranes without causing infection; however, overgrowth of these organisms can cause symptoms to develop. Symptoms of candidiasis vary depending on the area of the body that is infected.
1) Oral Thrush in Mouth or Throat
Candida yeasts normally live on the skin and mucous membranes without causing infection; however, overgrowth of these organisms can cause symptoms to develop. Symptoms of candidiasis vary depending on the area of the body that is infected.
1) Oral Thrush in Mouth or Throat
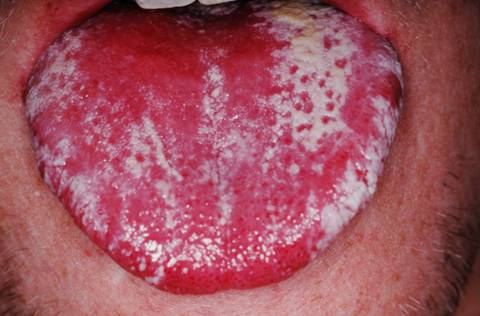
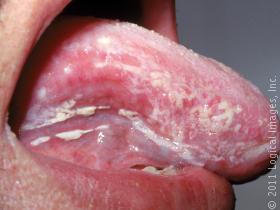
Candidiasis that develops in the mouth or throat is called “thrush” or oropharyngeal candidiasis.
The most common symptom of oral thrush is white patches or plaques on the tongue and other oral mucous membranes. This infection is uncommon among healthy adults.
Candidiasis of the mouth and throat, also known as “thrush" or oropharyngeal candidiasis, is a fungal infection that occurs when there is overgrowth of a yeast called Candida. Candida yeasts normally live on the skin or mucous membranes in small amounts. However, if the environment inside the mouth or throat becomes imbalanced, the yeasts can multiply and cause symptoms.
Candidiasis of the mouth and throat, also known as “thrush" or oropharyngeal candidiasis, is a fungal infection that occurs when there is overgrowth of a yeast called Candida. Candida yeasts normally live on the skin or mucous membranes in small amounts. However, if the environment inside the mouth or throat becomes imbalanced, the yeasts can multiply and cause symptoms.
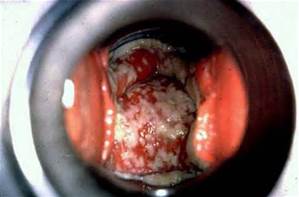
Candida overgrowth can also develop in the esophagus, and this is called Candida esophagitis, or esophageal candidiasis.
Candida infections of the mouth and throat can manifest in a variety of ways. The most common symptom of oral thrush is white patches or plaques on the tongue and other oral mucous membranes.
Other symptoms include:
Who Gets Oral Candidiasis?
Candida infections of the mouth and throat are uncommon among adults who are otherwise healthy. Oral thrush occurs most frequently among babies less than one month old, the elderly, and groups of people with weakened immune systems.
Other factors associated with oral and esophageal candidiasis include:
How Can I Prevent Oral Candidiasis?
Good oral hygiene practices may help to prevent oral thrush in people with weakened immune systems. Some studies have shown that chlorhexidine (CHX) mouthwash can help to prevent oral candidiasis in people undergoing cancer treatment.
Candida infections of the mouth and throat can manifest in a variety of ways. The most common symptom of oral thrush is white patches or plaques on the tongue and other oral mucous membranes.
Other symptoms include:
- Redness or soreness in the affected areas
- Difficulty swallowing
- Cracking at the corners of the mouth (angular cheilitis)
- It is important to see your doctor if you have any of these symptoms.
Who Gets Oral Candidiasis?
Candida infections of the mouth and throat are uncommon among adults who are otherwise healthy. Oral thrush occurs most frequently among babies less than one month old, the elderly, and groups of people with weakened immune systems.
Other factors associated with oral and esophageal candidiasis include:
- HIV/AIDS
- Cancer treatments
- Organ transplantation
- Diabetes
- Corticosteroid use
- Dentures
- Broad-spectrum antibiotic use
How Can I Prevent Oral Candidiasis?
Good oral hygiene practices may help to prevent oral thrush in people with weakened immune systems. Some studies have shown that chlorhexidine (CHX) mouthwash can help to prevent oral candidiasis in people undergoing cancer treatment.
2) Genital / vulvovaginal candidiasis (VVC)
Candidiasis in the vagina is commonly referred to
as a “yeast infection”
as a “yeast infection”
Genital / vulvovaginal candidiasis (VVC) is also sometimes called a "yeast infection," and it occurs when there is overgrowth of the normal yeast in the vagina. This infection is relatively common -- nearly 75% of all adult women have had at least one "yeast infection" in their lifetime.
Women with VVC usually experience genital itching, burning, and sometimes a "cottage cheese-like" vaginal discharge.
Women with VVC usually experience genital itching, burning, and sometimes a "cottage cheese-like" vaginal discharge.
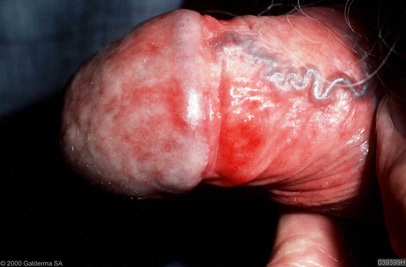
Men with genital candidiasis may experience an itchy rash on the penis.
The symptoms of VVC are similar to those of many other genital infections, so it is important to see your doctor if you have any of these symptoms.
Who Gets Genital / Vulvovaginal Candidiasis?
Nearly 75% of all adult women have had at least one "yeast infection" in their lifetime. On rare occasions, men can also get genital candidiasis. VVC occurs more frequently and more severely in people with weakened immune systems.
Other conditions that may put a woman at risk for genital candidiasis include:
How can I Prevent Genital / Vulvovaginal Candidiasis?
Wearing cotton underwear may help to reduce the risk of developing a yeast infection. For women who experience recurrent yeast infections (more than three per year), some evidence suggests that oral or intravaginal probiotics may help to prevent frequent infections.
3) Invasive Candidiasis
Who Gets Genital / Vulvovaginal Candidiasis?
Nearly 75% of all adult women have had at least one "yeast infection" in their lifetime. On rare occasions, men can also get genital candidiasis. VVC occurs more frequently and more severely in people with weakened immune systems.
Other conditions that may put a woman at risk for genital candidiasis include:
- Pregnancy
- Diabetes
- Long-term use of broad-spectrum antibiotics
- Use of corticosteroid medications
How can I Prevent Genital / Vulvovaginal Candidiasis?
Wearing cotton underwear may help to reduce the risk of developing a yeast infection. For women who experience recurrent yeast infections (more than three per year), some evidence suggests that oral or intravaginal probiotics may help to prevent frequent infections.
3) Invasive Candidiasis
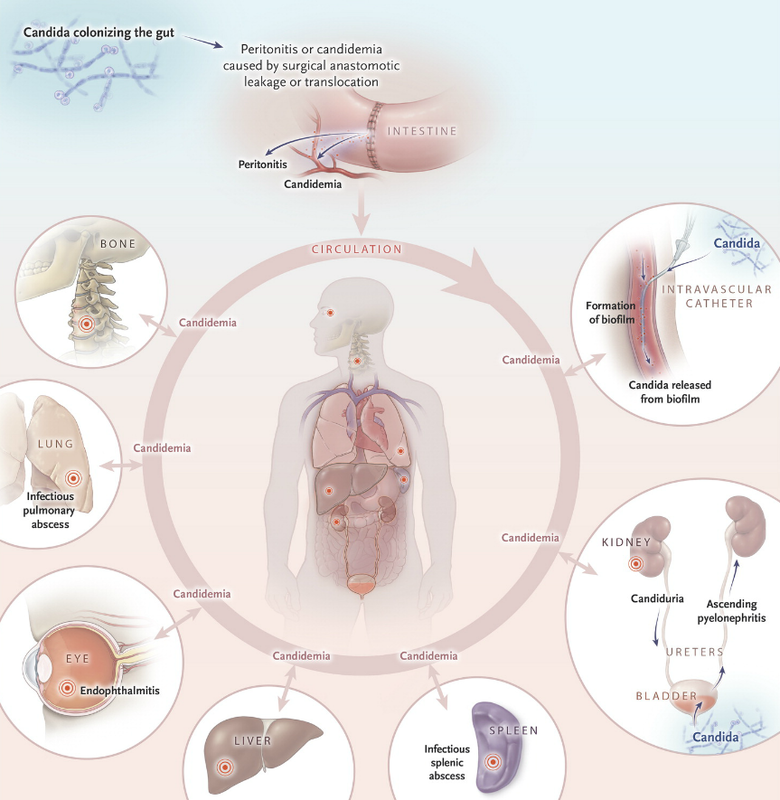
Invasive Candidiasis occurs when Candida species enter the bloodstream and spread throughout the body.
Invasive candidiasis is an infection caused by a yeast (a type of fungus) called Candida. Unlike Candida infections in the mouth and throat (also called “thrush”) or vaginal “yeast infections,” invasive candidiasis is a serious infection that can affect the blood, heart, brain, eyes, bones, and other parts of the body. Candidemia, a bloodstream infection with Candida, is a common infection in hospitalized patients.
Candida normally lives in the gastrointestinal tract and on skin without causing any problems. However, in certain patients who are at risk, Candida can enter the bloodstream and cause an infection.
A Candida bloodstream infection, which is the most common form of invasive candidiasis, is called candidemia, In the United States, candidemia is one of the most common causes of bloodstream infections in hospitalized patients, and it often results in long hospital stays, high medical costs, and poor outcomes.
People who develop invasive candidiasis are often already sick from other medical conditions, so it can be difficult to know which symptoms are related to a Candida infection. However, the most common symptoms of invasive candidiasis are fever and chills that don’t improve after antibiotic treatment for suspected bacterial infections. Other symptoms can develop if the infection spreads to other parts of the body, such as the heart, brain, eyes, bones, or joints.
Most cases of invasive candidiasis occur in people who have recently been admitted to a hospital or been in contact with other healthcare settings such as nursing homes.
People who are at high risk for developing invasive candidiasis include:
How to Prevent Invasive Candidiasis
Be a safe patient. There are some actions that you can take to help protect yourself from infections, including:
Speak up. Patients and caregivers can ask how long a central venous catheter is needed, and if so, how long it should stay in place. Tell your doctor if the skin around the catheter becomes red or painful.
A Candida bloodstream infection, which is the most common form of invasive candidiasis, is called candidemia, In the United States, candidemia is one of the most common causes of bloodstream infections in hospitalized patients, and it often results in long hospital stays, high medical costs, and poor outcomes.
People who develop invasive candidiasis are often already sick from other medical conditions, so it can be difficult to know which symptoms are related to a Candida infection. However, the most common symptoms of invasive candidiasis are fever and chills that don’t improve after antibiotic treatment for suspected bacterial infections. Other symptoms can develop if the infection spreads to other parts of the body, such as the heart, brain, eyes, bones, or joints.
Most cases of invasive candidiasis occur in people who have recently been admitted to a hospital or been in contact with other healthcare settings such as nursing homes.
People who are at high risk for developing invasive candidiasis include:
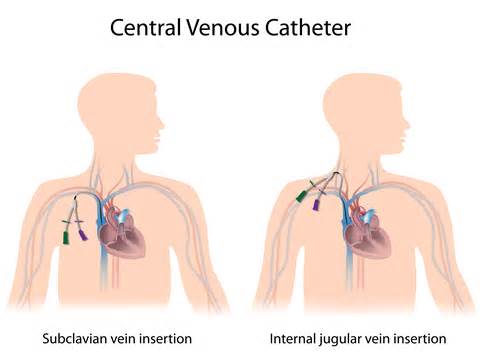
- Patients who have a central venous catheter
- Patients in the intensive care unit (ICU)
- People who have weakened immune systems (for example, people who have had an organ transplant, have HIV/AIDS, or are on cancer chemotherapy)
- People who have taken broad-spectrum antibiotics
- People who have a very low neutrophil (a type of white blood cell) count (neutropenia)
- People who have kidney failure or are on hemodialysis
- Patients who have had surgery, especially gastrointestinal surgery
- Patients who have diabetes
How to Prevent Invasive Candidiasis
Be a safe patient. There are some actions that you can take to help protect yourself from infections, including:
Speak up. Patients and caregivers can ask how long a central venous catheter is needed, and if so, how long it should stay in place. Tell your doctor if the skin around the catheter becomes red or painful.
Keep hands clean. Be sure everyone cleans their hands before touching you. Washing hands can prevent the spread of germs.
Eating Healthily to avoid/prevent/reduce Candidiasis.
Many foods can make us vulnerable to Candidiasis. To thoroughly avoid them is easier said than done. If you already suffer from the infection, it is best to avoid them. If you are infection free but know you're prone to recurrent Candidiasis, then you need to maintain a healthy balance and have these foods with care and moderation.
Foods to Try to Have More of, to Prevent Candida:
To prevent Candidiasis, foods to have with caution are:
- Whole wheat, whole bread products.
- Drink milk and have more of yogurts rich in lactobacilli, a normally occurring gut bacterium which keeps a check on Candida growth.
- Garlic is known to have natural anti-fungal properties.
To prevent Candidiasis, foods to have with caution are:
- Foods high in sugars - cakes, pastries, jams, syrups, canned syrups, chocolate, honey, molasses, biscuits, puddings, marzipan, ice-creams, soft-drinks etc. Many food packages even disguise presence of sugars by using terms like sucrose, dextrose, fructose, lactose etc. In short, sugar in any form is best avoided! Even artificial sweeteners are equally harmful.
- Fermented foods like beer, cider, wine, pickles, etc. Alcohols eventually get converted into sugar thus in increase the sugar content in the blood stream allowing Candida to grow.
- Refined food products like white pasta, cornflakes, white rice, custard powder etc.
- Nuts. Most nuts are very moldy. Hence, if you have Candidiasis, avoid nuts.
- Tea, coffee, hot chocolates or any malted drinks (e.g. horlicks).
THE CANDIDA DIET
Many Complementary and Alternative Medicine (CAM) Practitioners advocate that patients who suspect they may be suffering from Candida follow the Candida Diet for a specific period of time, anywhere from three to six months.
Key aspects of the diet include:
• The removal of sugar: Yeast-like Candida feed off of sugar – even foods that your body converts into sugar, such as simple carbohydrates (fruit, potatoes, white rice and pasta). This makes the diet challenging because you have to stick to eating mostly protein and vegetables.
• Avoiding fermented foods: Mushrooms, vinegars, most condiments, and even cantaloupe can also contribute to the growth of yeast.
• Avoiding other trigger foods: aged and mouldy cheeses, foods that contain yeast or moulds (most breads, muffins, baked goods), honey, syrups and glutinous foods such as barley, oats, wheat and rye.
• The introduction of a probiotic such as acidophilus to help restore the balance of bacteria in the body, especially in the gastrointestinal system.
Many Complementary and Alternative Medicine (CAM) Practitioners advocate that patients who suspect they may be suffering from Candida follow the Candida Diet for a specific period of time, anywhere from three to six months.
Key aspects of the diet include:
• The removal of sugar: Yeast-like Candida feed off of sugar – even foods that your body converts into sugar, such as simple carbohydrates (fruit, potatoes, white rice and pasta). This makes the diet challenging because you have to stick to eating mostly protein and vegetables.
• Avoiding fermented foods: Mushrooms, vinegars, most condiments, and even cantaloupe can also contribute to the growth of yeast.
• Avoiding other trigger foods: aged and mouldy cheeses, foods that contain yeast or moulds (most breads, muffins, baked goods), honey, syrups and glutinous foods such as barley, oats, wheat and rye.
• The introduction of a probiotic such as acidophilus to help restore the balance of bacteria in the body, especially in the gastrointestinal system.
Sanitation is Important for Preventing Candidiasis
The importance of maintaining a high standard of
Personal Hygiene cannot be disregarded.
Personal Hygiene cannot be disregarded.
- Wear loose clothes and undergarments, must have a cotton crotch.
- After toilet, wipe from front to back only. This prevents contamination of the vagina with anal microorganisms.
- Maintain good oral hygiene. Brush twice daily, especially in the night within four hours after meals. Floss regularly (at least twice a week) or use mouthwashes. Try using warm, salted-water gargles to relive mouth & throat symptoms.
- Keep the vaginal area always dry. Especially after a bath or shower. Be sure to wash the area thoroughly when in a bath or shower. Avoid very strong soaps.
- If you exercise or swim, change out of the clothes immediately after the workout.
- Douching should be avoided.
- Avoid using highly perfumed scents or soaps.
- Undergarments must be washed in warm water and softeners should be used sparingly.
- Scented sanitary pads or tampons are best avoided. Change the pads frequently, keeping the area dry.
- Avoid sharing towels, razors and other toiletries.
- Practice safe sex to prevent getting or spreading Candidiasis
Genital Candidiasis often spreads through infected sexual partners. Often both partners need to undergo treatment.
Both partners should clean themselves before and after having sex.
Use a condom if either partner is infected or undergoing treatment.
Avoid vaginal sex immediately after anal sex and never without washing.
Use lubricants when the natural secretions are insufficient.
Always use water based lubricants only.
Ease up on your medications to avoid Candidiasis
Use a condom if either partner is infected or undergoing treatment.
Avoid vaginal sex immediately after anal sex and never without washing.
Use lubricants when the natural secretions are insufficient.
Always use water based lubricants only.
Ease up on your medications to avoid Candidiasis
Indiscriminate use of antibiotics can gradually make the bacteria resistant to them. Thus, very often you end up using more and more potent antibiotics. You really do not need an antibiotic for that cold or tummy ache. Frequent antibiotic usage kills other organisms that compete with Candida and help its growth.
Besides, all antibiotics come with their own share of side-effects.
So, stop popping pills at the drop of a hat!
Besides, all antibiotics come with their own share of side-effects.
So, stop popping pills at the drop of a hat!
Women suffering from Candidiasis must find alternatives for their contraception. Check with your doctor before having pills to avoid pregnancy.
Also check with your physician to find suitable nutritional supplements.
HOW HOMEOPATHY CAN HELP
My experience is that the Candida Diet can be very successful for cases of mild to moderate Candida. In fact, dietary changes are often a necessary part of decreasing and eliminating symptoms of Candida. However, I treat a lot of patients with Candida and repeatedly hear how the Candida diet did not alleviate or remove their symptoms completely. For many people, systemic Candida infection cannot be resolved by diet alone. This is where homeopathy can be very useful.
Homeopathic medicine is holistic because it takes into consideration your unique experience of disease on the mental, emotional and physical levels.
As a Homeopath, I want to know whether you are prone to chronic yeast infections including oral Candida (thrush), as well as many of the other possible associated symptoms of Candida. For example, if you get chronic yeast infections, when do you get them, what do they feel like (do they itch, burn, sting?) and what does this discharge look like. Homeopaths are also fundamentally interested in you as a person. We ask questions about your body temperature, how weather affects you, patterns of perspiration, sleep, digestion and much more.
In most cases, the selection of a homeopathic remedy for you will also help to address other chronic health issues that have been bothering you such as migraines, constipation, PMS or anxiety / depression.
HOMEOPATHIC REMEDIES FOR CANDIDA
Also check with your physician to find suitable nutritional supplements.
HOW HOMEOPATHY CAN HELP
My experience is that the Candida Diet can be very successful for cases of mild to moderate Candida. In fact, dietary changes are often a necessary part of decreasing and eliminating symptoms of Candida. However, I treat a lot of patients with Candida and repeatedly hear how the Candida diet did not alleviate or remove their symptoms completely. For many people, systemic Candida infection cannot be resolved by diet alone. This is where homeopathy can be very useful.
Homeopathic medicine is holistic because it takes into consideration your unique experience of disease on the mental, emotional and physical levels.
As a Homeopath, I want to know whether you are prone to chronic yeast infections including oral Candida (thrush), as well as many of the other possible associated symptoms of Candida. For example, if you get chronic yeast infections, when do you get them, what do they feel like (do they itch, burn, sting?) and what does this discharge look like. Homeopaths are also fundamentally interested in you as a person. We ask questions about your body temperature, how weather affects you, patterns of perspiration, sleep, digestion and much more.
In most cases, the selection of a homeopathic remedy for you will also help to address other chronic health issues that have been bothering you such as migraines, constipation, PMS or anxiety / depression.
HOMEOPATHIC REMEDIES FOR CANDIDA
Homeopathy works by prescribing one remedy that is the closest match for your symptoms of Candida. This means there are many remedies that can help. Furthermore, each person with Candida may have more symptoms than just yeast infections that a Homeopath will take into consideration.
|
|
|
|